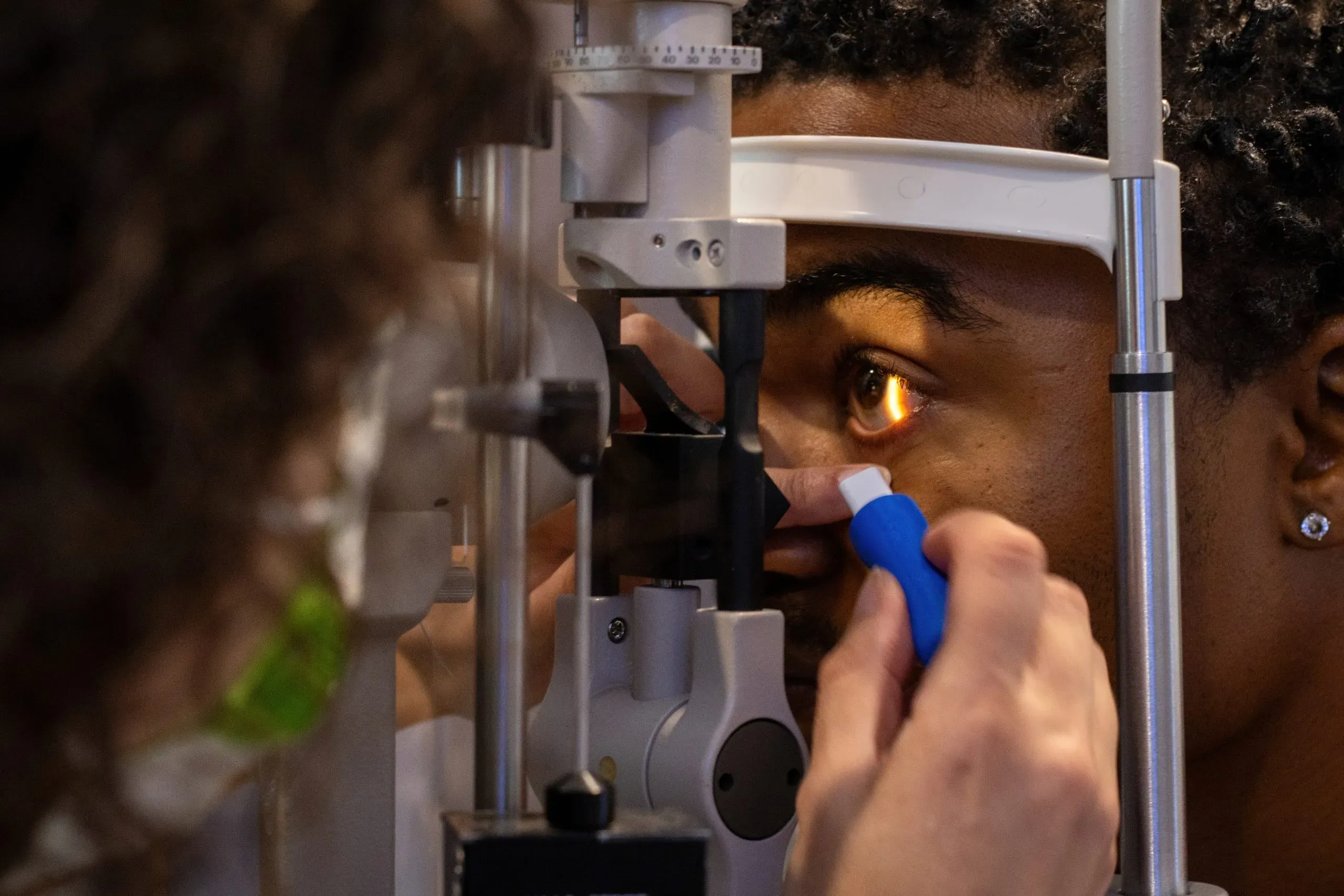
Diabetic retinopathy refers to several eye problems that are characterized by damage to the light-sensitive retina, caused by excessive blood sugar levels. Almost half of Americans with diabetes suffer from some level of diabetic retinopathy. When glucose levels in the blood are not properly controlled, it can result in the formation of glaucoma, cataracts or blood vessel damage in the retina — all of which can cause vision loss if not diagnosed and treated early.
Damage to the blood vessels in the retina can eventually lead to permanent vision loss. High blood sugar levels can lead to the blood vessels in the retina swelling and leaking. This leaked blood in the eye damages vision. In severe instances, the retina can thicken and crack, causing new blood vessels to grow under the retina and through those cracks, which severely affects visual acuity.
Symptoms
For many people, the earliest stages of diabetic retinopathy do not have any easily noticeable symptoms. By the time vision loss is prominent enough to be noticed, most individuals have progressed to advanced stages of diabetic retinopathy that are harder to treat and manage.
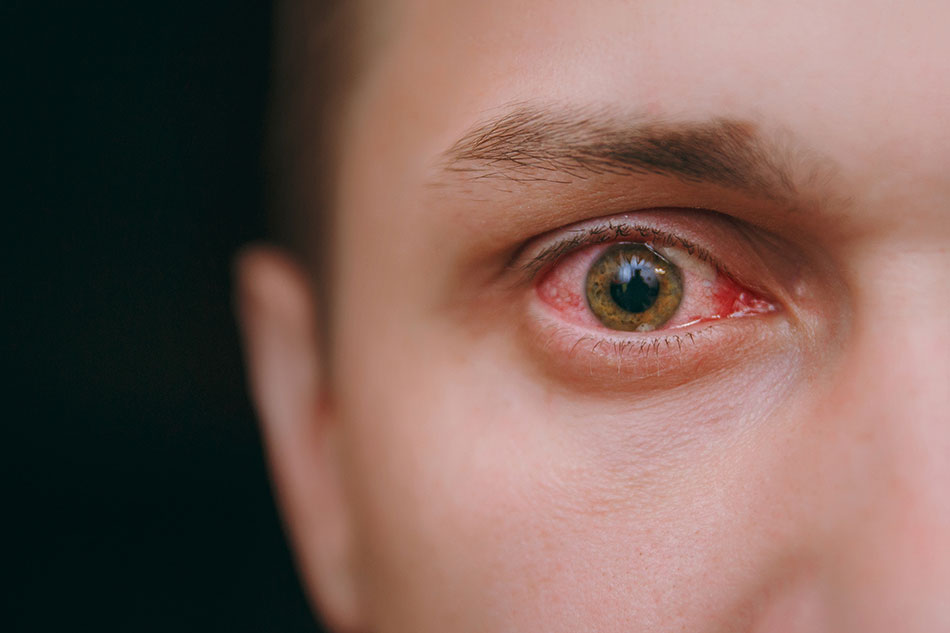
Thankfully, regular eye examinations can help monitor the eyes for many of the common initial warning signs of diabetic retinopathy, including the following:
- Floaters or spots roaming around in your field of vision
- Poor night vision
- An empty or dark spot in the middle of your field of vision
- Blurred vision
Treatment
Treatment of diabetic retinopathy depends on the stage and severity of the condition. Through regular eye examinations and pupil dilation, diabetic retinopathy can be monitored closely to ensure accurate treatment. Keeping blood sugar levels within recommended ranges can also help manage or slow the progression of diabetic retinopathy.
In more severe cases, treatment also includes:
- Laser surgery to repair retinal detachment
- Intravitreal injections of medications into the jelly-like vitreous, near the retina, to stop the proliferation of blood vessels and halt further retinal damage
- Laser photocoagulation (to close leaking blood vessels in the retina)
Reduce Your Risk
Between 40 and 45 percent of all diabetic patients have some form of diabetic retinopathy, but there are some actions you can take to reduce your likelihood of developing the condition.
If you have diabetes, it is important to regularly check your blood sugar levels and take steps to keep those levels within the normal range. Individuals with diabetes should also receive regular eye exams. For many people, having an eye exam once a year is generally considered sufficient. However, some individuals, such as those with diabetes and consequent eye concerns, may need to visit their eye doctor and undergo eye exams more frequently.
Want to Know More?
If you have additional questions about diabetic retinopathy or think you are experiencing some of the symptoms, please contact us for more information or to schedule an appointment.